- +91 - 90 6646 2996 | 90 6636 2996
- +91 - 40 - 2330 2996 | 40 - 2335 0696
- drraghuveerreddy3@gmail.com
Shoulder Arthritis
Arthritis implies inflammation of a joint, but in common usage usually means wearing out of that joint - either the joint surfaces (cartilage) or the muscles and capsule of that joint have degenerated.
Symptoms
- Grating with joint movement as the joint surfaces are irregular.
- Night pain due to the accompanying inflammation-a reaction to the wear & tear particles within the joint over a life time.
- Movement restriction as the capsule has shrunk and the joint is too painful to move because of above.
Investigations
- X-rays show the changes in the bone structures and the "joint" space between the bones.
- CT.Scan: may show the 3 dimensional structure of the bones and the state of the muscles - whether replaced by fat or good contracting muscle which will work to move the joint after a joint replacement.
- MRI: also to show the state of the muscles to predict the eventual functional recovery after a shoulder joint replacement.
Treatments
Conservative
- Anti inflammatory tablets
- Physiotherapy: to reduce inflammation, maintain movement and muscle status.
- Cortisone (or hydrocortisone or steroid) injections into the joint may help to settle a flare up of the arthritis.
Operative - Minimally Invasive
This procedure is done with the arthroscope to remove any loose bodies, any cartilage flaps,inflamed synovium (joint lining). Noxious enzymes or wear particles can be washed out of the joint. Postoperatively the patients are encouraged to undergo a rehabilitation programme.
SHOULDER ARTHROPLASTY
When severe shoulder pain starts interfering with daily activities, it may be time to consider surgical options designed to provide pain relief and freedom of movement. Over 60,000 Americans have shoulder replacement procedures each year, many experiencing pain relief and improved function. An increasing number of patients are returning to more active lifestyles thanks to advancements in the materials and procedures used in shoulder replacement. Today, shoulder replacement is the third most common joint replacement. In a study of patients with shoulder pain, more than 95% reported having less pain after shoulder replacement.
What makes up to a total shoulder replacement?
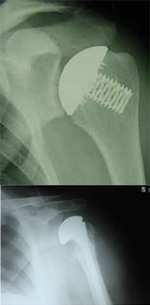 In total shoulder replacement surgery, the ball of the humerus and socket of the scapula (glenoid) are replaced with specially designed components.
In total shoulder replacement surgery, the ball of the humerus and socket of the scapula (glenoid) are replaced with specially designed components.
The humeral implant consists of a metal ball that replaces the head of the humerus, and a stem that is secured into the main arm bone (humerus).
The humeral stem is made of titanium for maximum strength. The head is made of cobalt chrome to provide a smooth surface for movement with the glenoid component, which is made of medical-grade polyethylene.
The metal ball and stem are selected by the surgeon from multiple sizes to fit the contour and shape of each patient?s humerus. This two-piece construction is known as a modular implant. This modularity allows surgeons to closely replicate the natural shoulder. If the surgeon uses only the metal humeral components (humeral head and stem), the procedure is called a partial shoulder replacement. If the surgeon uses both the humeral components and the glenoid implant, the procedure is called a total shoulder replacement. Surgeons will decide which procedure to use based on the extent of damage to their patients? shoulders.
The goal of shoulder replacement arthroplasty is to restore the best possible function to the joint by removing scar tissue, balancing muscles, and replacing the destroyed joint surfaces with artificial ones.
Reverse Shoulder Arthroplasty
The reverse shoulder arthroplasty has provided an innovative and effective way to relieve pain and restore function in many patients with rotator cuff deficiencies,"
Rationale, advantages, disadvantages
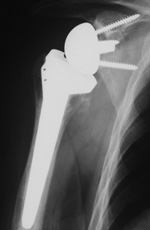 RSA reverses the natural anatomy of the ball-and-socket joint by implanting a concave socket plate into the humeral head and a convex spherical glenoid component into the glenoid fossa. RSA also treats arthritis by resurfacing the glenohumeral joint.
RSA reverses the natural anatomy of the ball-and-socket joint by implanting a concave socket plate into the humeral head and a convex spherical glenoid component into the glenoid fossa. RSA also treats arthritis by resurfacing the glenohumeral joint.
The goal is to reduce pain and restore function by overcoming vulnerabilities of traditional shoulder replacements in which the absence of a stabilizing rotator cuff can lead to poor function and mechanical failure of the implant.
By reversing the anatomy, the surgery improves deltoid tension and provides a stable fulcrum that compensates for loss of rotator cuff performance. In the absence of a rotator cuff, attempted arm elevation results in superior migration of the humeral head, with no real fulcrum and poor motion.
With RSA, the constrained nature of the implant provides a fulcrum that is particularly advantageous for a better tensioned deltoid.
Reverse shoulder arthroplasty advantages and disadvantages
RSA advantages include
- More consistent pain relief due to replacing both sides of the joint, an advantage over hemiarthroplasty
- Restoration of active elevation
- Improved shoulder stability
Indications
The primary indication for a reverse total shoulder replacement is for rotator cuff arthropathy. This is a condition of progressive arthritic degeneration of the shoulder joint due to longstanding rotator cuff dysfunction as a result of chronic rotator cuff tears within the shoulder. At least two of the four rotator cuff muscles (supraspinatus, infraspinatus, teres minor and subscapularis) need to be torn or dysfunctional in order to develop rotator cuff arthropathy. As a result of the dysfunction, the normal biomechanics of the shoulder joint are lost. The pathologic mechanics of the shoulder joint lead to the eventual development of disabling arthritic change of the shoulder. This condition is termed rotator cuff arthropathy. This prosthesis is ideally suited for the older patient with lower functional demands with significant functional limitations as a result of this condition.
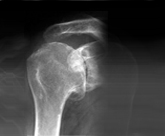
A radiograph of the shoulder showing a high riding humeral head. This suggests a chronic irreparable rotator cuff tear.
